HealthLock Membership
HealthLock automatically reviews your medical claims and flags medical bill errors to help you save. Your membership covers your entire family, even if you have different insurance coverage.
$19.99/month
We work around the clock to monitor your providers for HIPAA violations and breaches of your private medical information. When we detect a breach at one of your providers, we’ll alert you.
If you don’t recognize a doctor or your bill doesn’t match, just let us know. We’ll investigate to uncover whether it’s an error or a misuse of your information. If it’s fraud, our team will help fix the problem.
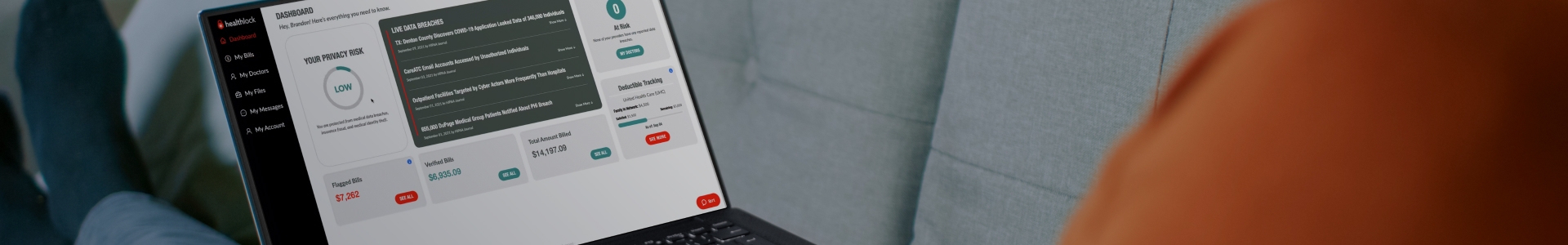
The only score of its kind, we calculate your privacy exposure based on several risk factors. As the score changes, we alert you via your dashboard so you can take control of your medical privacy.
We alert you by email or text whenever we detect new claims, a breach, or a potential threat. Our comprehensive alerts provide expanded notifications for our enhanced plans to help you stop medical and financial identity theft early.
See all your medical claims at a glance. We bring all your insurance-submitted doctor and medical service claims into a single location for easy review and verification.
Using our powerful HealthLock DeepAudit Technology, we automatically audit incoming claims and flag potential upcoding and overcharges so you can get your money back.
Take back control of your healthcare with our centralized, easy-to-understand dashboard. View your claims, deductibles, doctors, and more on your desktop or mobile phone. Securely upload your insurance cards, invoices, and receipts for easy access anytime.
Have a question? Our friendly team of knowledgeable experts is available via email or chat to provide advice and answer your questions about alerts, your dashboard, and your membership.
Upon joining, we’ll analyze up to two years of your previous medical claims and flag potential overcharges using our HealthLock DeepAudit technology. While in most cases these claims are past the 90-day window for negotiation, the analysis helps you identify the potential for future overbilling issues.
For select flagged bills that are less than 90 days old, you can elect to have us work on your behalf to reclaim money from overbilled and overpaid bills.
Track what medical expenses you’ve paid out-of-pocket already and know how much you have left to meet your annual deductibles.
If you’ve been overcharged by a provider, you can request that we negotiate on your behalf to help get your money back. To date, we’ve helped our members save over $130 million.
When we negotiate on your behalf, we’ll assign you to a Personal Reimbursement Specialist. While our team is busy getting your money back, they’ll be your point of contact.
Stop overpaying for healthcare. Start saving today.
$19.99/month
* Remediation includes guidance throughout the recovery process, assistance in restoring accuracy to credit reports and medical records, help reporting errors to health care providers, and assistance finding new doctors.
§ Negotiation and recovery services require 20% shared savings of reclaimed money or bill reduction, charged to the payment option on file upon confirmation of recovery from the carrier or provider. Example: You request our help with a claim or bill, HealthLock successfully appeals the claim, you receive a reimbursement check of $300 from your insurance and HealthLock charges you a $60 Shared Savings fee.
† Historical Claim Analysis and 90-day Retro Audit and Recovery are provided once per member lifetime only during initial enrollment.
1 KFF, the independent source for health policy research, polling and news.
